|
6/23/2016
Creating Self-Healing Neurons
By Niharika Vattikonda
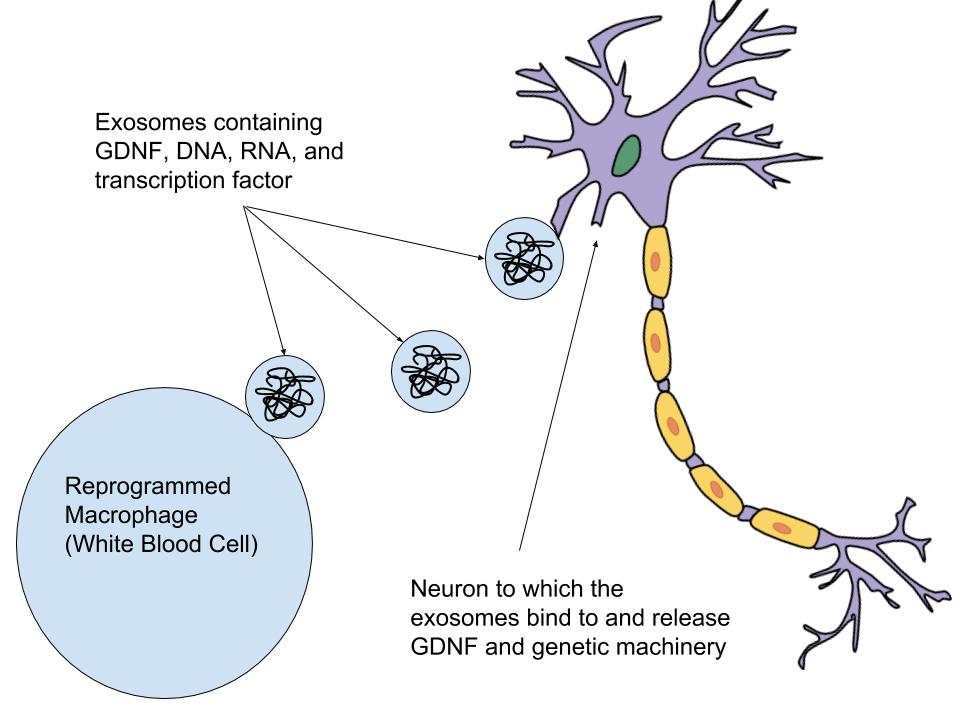
What if we could heal ourselves? The question seems to be straight out of a supernatural fantasy, but recently, a team of researchers at the University of North Carolina at Chapel Hill has proved that we are not very far. Led by Dr. Elena Batrakova, the research group created “smarter” immune cells to be delivered to the brain for healing damaged neurons. These immune cells produce and deliver a protein that heals the brain while “teaching” the affected neurons how to continue making that protein for themselves. This groundbreaking research could prove useful in reversing the brain cell damage caused by Parkinson’s disease - a neurodegenerative brain disorder in which the affected individual gradually loses his/her ability to regulate movements and emotions. The disability is caused by low amounts of dopamine - a key neurotransmitter present in brain cell neurons. Due to death of its parent cells - 60-80% death in a midbrain region called substantia nigra - the production of dopamine is slowed down substantially, disturbing daily life in the affected. Dopamine is a neurotransmitter that is responsible for reward-driven behavioral effects. While only relatively few neurons are dopaminergenic (only about 400,000), if cells survive, dopamine production is able to proceed at a normal rate. During Parkinson’s disease, these cells undergo apoptosis (cell death) and dopamine production staggers. The disease itself is not fatal. However, the Centers for Disease Control and Prevention (CDC) have noted that complications from the disorder are the 14th highest cause of death within the United States. Smart immune cells were genetically modified macrophages (white blood cells) and seem to help the cells that are undergoing damage and stop further damage to rest of the neurons (20 – 40%). Although the smart immune cells have yet to show whether they are able to replenish the dopamine lost by cell death, by preventing more cells from dying, these immune cells could stabilize dopamine production, slowing the progression of the disease. The treatment would go beyond the current therapies aimed at addressing the patient’s life quality through dopamine replacement, as no such treatment exists now that could halt Parkinson’s disease. The key to making this a successful treatment is the use of repurposed white blood cells, which avoid the body’s immune response and are able to penetrate the blood-brain barrier. Most medicines cannot achieve the later. Once the reprogrammed cells are in the brain, they produce and release exosomes - tiny membrane-bound pockets containing glial cell-derived neurotrophic factor (GDNF). GDNF is a growth factor or protein that is naturally occurring in the brain and promotes the survival of neurons in the central and peripheral nervous systems, particularly motor neurons and midbrain dopaminergenic neurons. The released exosomes can then travel and bind to neurons in the brain, releasing the GDNF. Past research has shown that the GDNF delivered to the brain can possibly increase the survival rate of neurons in the substantia nigra, which could ultimately slow and potentially reverse the progression of Parkinson’s disease. Dr. Batrakova’s research has successfully proved it now. The “teaching” factor, however, is arguably one of the most critical points of the treatment. Although the bioengineered white blood cells deliver the GDNF directly to the neurons, in order to ensure that the treatment has a long-term effect in halting or reversing Parkinson’s disease, the tools and instructions for creating the protein are also delivered. This toolkit containing DNA, messenger RNA, and transcription factor enable the neurons to synthesize the protein, GDNF, using their own transcription and translation processes, which do not rely on constant delivery of the protein via the engineered macrophages. Batrakova said, “By teaching immune systems to make this protective protein, we harness the natural systems of the body to combat degenerative conditions like Parkinson’s disease.” In order to develop this amazing technology into a viable treatment, the North Carolina Biotechnology Center awarded Batrakova and her researchers with a $50,000 Technology Enhancement grant, with the belief that “we will see these discoveries on the frontiers of scientific moving into clinical practice,” said Alexander Kabanov, director of the nanotechnology center. Although this technology is only in the earliest stages of commercial development, it is likely that this will become one of the major ways that we treat and eventually eradicate Parkinson’s disease.
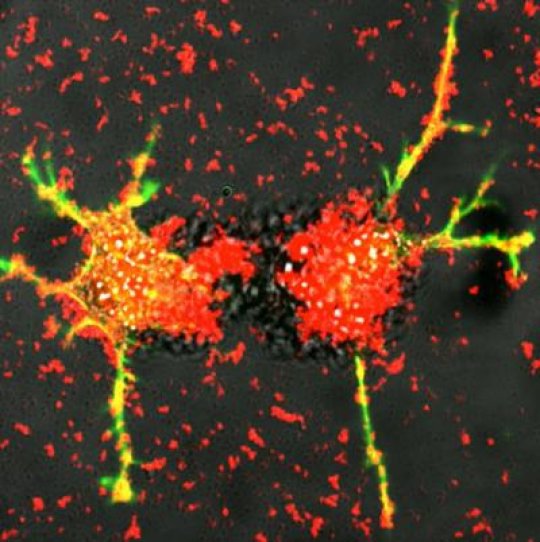
Image: Bioengineered white blood cells (macrophages) that contain the glial cell-derived neurotrophic factor and the molecular machinery to “teach” neurons how to produce the protein. (Credit: Elena Batrakova/UNC) 
About the Author
Niharika Vattikonda is currently a sophomore at Thomas Jefferson High School for Science and Technology in Northern Virginia – she loves biology and computer science. She recently completed a yearlong freshman research project on the effect of electromagnetic fields on E. coli. She first was exposed to Computer Science in middle school, when she learned coding in HTML/CSS, studied Java in freshman year, and is now learning app development on her own. Niharika enjoys STEM outreach, starting science clubs for girls at elementary schools and volunteering at science fairs and hackathons. When she’s not coding or writing for Scientista, Niharika enjoys debating, participating in Model United Nations, singing, and writing for her own blog, Teen Thoughts on Politics. Comments? Leave them below! |
Archives
February 2023
DiscovHER BlogScientista DiscovHER is a blog dedicated to discovHERies made by women in science. Follow us for links to the latest resHERch! Categories
All Alexandra Brumberg Amy Chan Avneet Soin Chemistry Diana Crow Engineering Health/medicine Indulekha Karunakaran Iqra Naveed Johanna Weker Lidiya Angelova Michael Clausen Mind Brain And Behavior Muhammad Hamza Waseem Nikarika Vattikonda Opinion Prishita Maheshwari-Aplin Technology Uma Chandrasekaran |
The Network for Pre-Professional Women in Science and Engineering
The Scientista Foundation is a registered 501(c)(3) -- Donate!

 RSS Feed
RSS Feed