|
By Michael Clausen
October is known for something other than Halloween. News articles, magazine stories, and blog posts are now out advertising Breast Cancer Awareness Month; a chance to learn more about the devastating disease and to donate in support of the cause. But this month, I invite you to reflect on whether we’re going about breast cancer in the wrong way.
Breast cancer awareness is pretty much universal by now. It’s become one of the medicine’s most wanted, but the medical and ethical complexities of breast cancer have clearly been drowned out by a one-dimensional race for the cure.
If there’s any word to change your thinking on the disease, it might just be “overdetection”. Overdetection means diagnosing a disease in people that doesn’t actually pose any threat to their life – it either isn’t malignant or it progresses too slowly. Overdetection is the single most harmful effect of cancer screening. Everybody is at risk for overdetection. But it can become an issue, especially for elderly patients and for those who already have a life-threatening disease and whose cancer might never be harmful in their lifetime. Many of these patients would die even before their cancer ever affects them. On all fronts, overdetection is a bad thing: it can mean costly insurance policy changes, taxing treatments like chemotherapy, extreme pressure on families of the “affected”, the psychological weight of a “cancer patient” label, and more. Enter Ann Van den Bruel – Associate Professor and Director of the National Institute for Health Research’s Diagnostic Evidence Cooperative at Oxford. Van den Bruel and her colleagues published a study last March that surveyed 1000 people in the UK about overdetection. Respondents were presented with two hypothetical scenarios. In both of them, there exists a population of 1000 people. Five percent (50) of them have cancer and one percent (out of 50 cases) will die from it. Any person can be screened for cancer, and screening will reduce deaths by 10% in the first scenario and 50% in the second scenario. For both scenarios, respondents were asked how many cases of overdetection they would be willing to accept (any number between and including 0 to 1000). Survey results showed no consensus, which the authors discussed in a recent publication (video below). The responses went something like this. Response 1: Some said that even one case of overdetection was too much. They might think, “The idea of having to go through cancer or chemo for something that would never harm me…that is so devastating to me,” says Van den Bruel. Response 2: “Some others really wanted to accept a huge number of overdetection, like the entire population,” says Van den Bruel. “Because for them, nothing was too costly…to avoid getting cancer. ” Response 3: Others held that overdetection in the entire population was acceptable if it meant no one had to suffer from cancer. “Well I have seen my mother die from breast cancer or I had a very good friend die from bowel cancer…and having witnessed that, I would want to go very far from ending up in that…situation.’” It’s clearly not an easy question. But overall, more people (13.9%) were willing to accept breast cancer overdetection in the entire population (response 2) than those (3.5%) who wouldn’t accept any overdetection at all (response 1)
Part of the discrepancy lies in the fact that overdetection is an incredibly abstract concept.
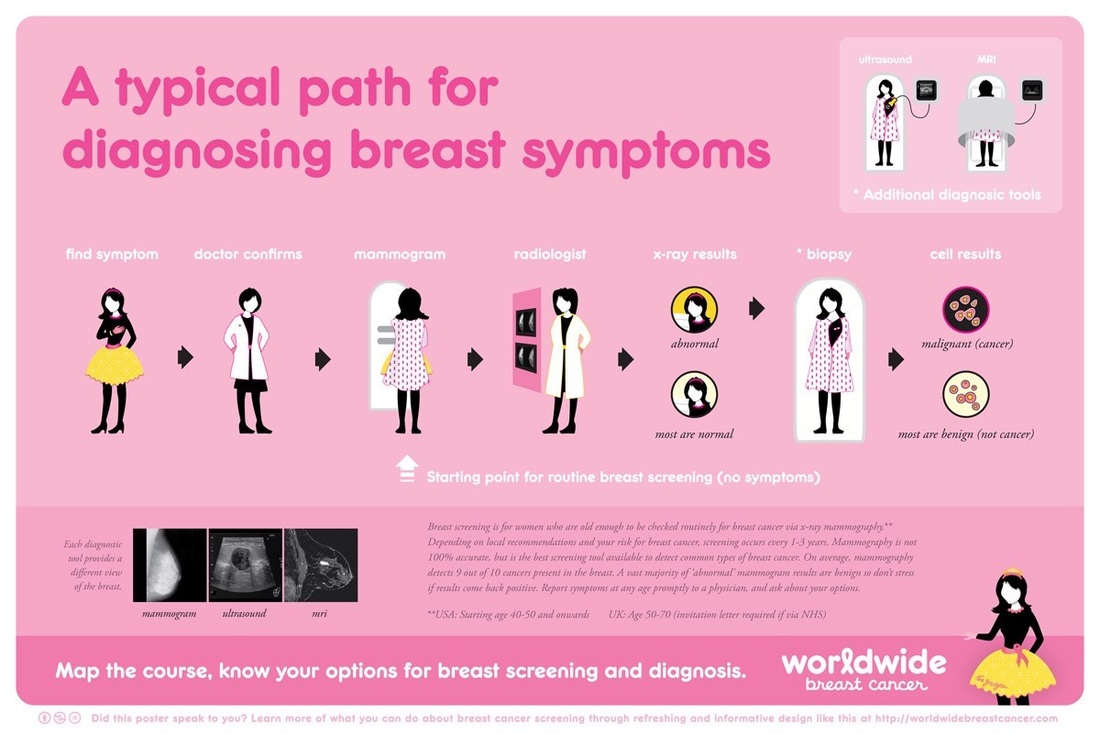
First, it’s not clear how many cases of overdetection really occur. One notable study published in 2012 suggested that over the last 30 years, breast cancer has been overdetected in 1.3 million women in the U.S. alone. The study also places 2008’s rate of overdetection as high as 31%. Others are dubious of so high an incidence rate. On the other hand, it’s hard to be exact. That’s because you can’t just count cases: it’s impossible to tell if any one patient is being overdetected. “It is not a question of whether we are detecting things that aren’t really cancer. The lesion is a cancer lesion,” says Van den Bruel. “But we just can’t know in an individual whether that lesion will grow very fast and then become threatening to that person’s health or whether that lesion is going to stay or grow very slowly and the person will eventually die from another cause.” If this all is hard to wrap your head around, you’re not alone. The survey respondents also felt that the concept of overdetection was really difficult to understand. Van den Bruel believes it takes time for patients to think it through. But beyond that, knowing about overdetection puts everybody between a rock and a hard place. There is a typical path for diagnosing breast cancer (see image below) and any positive invasive cancer screening might be just that: a truly malignant threat. But it may actually be a case of overdetection, potentially throwing any patient into a treatment they don’t need to endure. Of course they’d never know: their doctor can’t tell the difference between an overdetected and a rightfully detected cancer. This is the problem that overdetection presents. It forces individual people to weigh the costs and benefits of cancer screening, something we usually consider to be universally beneficial. Van den Bruel thinks that “we should be much more realistic about the fact that progression is variable. Some people have a cancer that doesn’t progress at all. And finding these early stage cancers is not always more beneficial than just waiting for symptoms to occur because in some cases, you still have plenty of time.” Overdetection should make everyone think twice about whether to be screened and treated for cancer. At the same time, it doesn’t negate the fact that breast cancer is a very serious and very emotional disease. What’s clear to me now is that in light of overdetection, everybody is forced to make an impossible decision: should I get screened – or not? —————-- References: Bleyer A, Welch, HG. Effect of three decades of screening mammography on breast-cancer incidence. New England Journal of Medicine 367.21 (2012): 1998–2005. Van den Bruel A, Jones C, Yang Y, Oke J, Hewitson P. People’s willingness to accept overdetection in cancer screening: population survey. BMJ 350 (2015): h980. 
About the Author
Michael Clausen is an undergraduate student studying linguistics at Pomona College in Claremont, CA. He is an amateur science writer with an interest in accurate representations of science in communication and the media. Michael is also a Curator at TEDxClaremontColleges, where he co-produces an independently organized TED-style conference. He was born and raised in Connecticut and is an avid cyclist. Comments? Leave them below! |
Archives
February 2023
DiscovHER BlogScientista DiscovHER is a blog dedicated to discovHERies made by women in science. Follow us for links to the latest resHERch! Categories
All Alexandra Brumberg Amy Chan Avneet Soin Chemistry Diana Crow Engineering Health/medicine Indulekha Karunakaran Iqra Naveed Johanna Weker Lidiya Angelova Michael Clausen Mind Brain And Behavior Muhammad Hamza Waseem Nikarika Vattikonda Opinion Prishita Maheshwari-Aplin Technology Uma Chandrasekaran |
The Network for Pre-Professional Women in Science and Engineering
The Scientista Foundation is a registered 501(c)(3) -- Donate!



 RSS Feed
RSS Feed